3 Tips to Build CPR Readiness in Athletics
Empower your team to perform confidently under pressure.

Empower your team to perform confidently under pressure.

If you work an athletic program, you likely know that safety planning is often framed around the Emergency Action Plan, or EAP. The EAP is a carefully designed roadmap that outlines who does what, when, and how during a medical emergency. But even the most well-written EAP is only as effective as the people executing it.
When sudden cardiac arrest (SCA) occurs, preparation must extend beyond policies and paperwork to include consistent, high-quality CPR and AED skills practiced in realistic conditions.
In this article, we share 3 tips for ensuring that your training program is effectively preparing your team to execute the EAP in the case of a SCA.
Most instances of sudden cardiac arrest in young athletes stem from inherited heart conditions that often remain undetected.2 Onset is often immediate and unforgiving. Survival depends on a rapid chain of events that includes early recognition, immediate CPR, and rapid defibrillation.
Most athletic departments recognize this reality and have AEDs strategically placed throughout facilities. Many also maintain venue-specific EAPs. However, in an actual emergency, equipment availability and written plans matter far less if responders lack confidence, coordination, or current skills.
This is where hands-on CPR and AED training becomes a cornerstone of emergency preparedness.
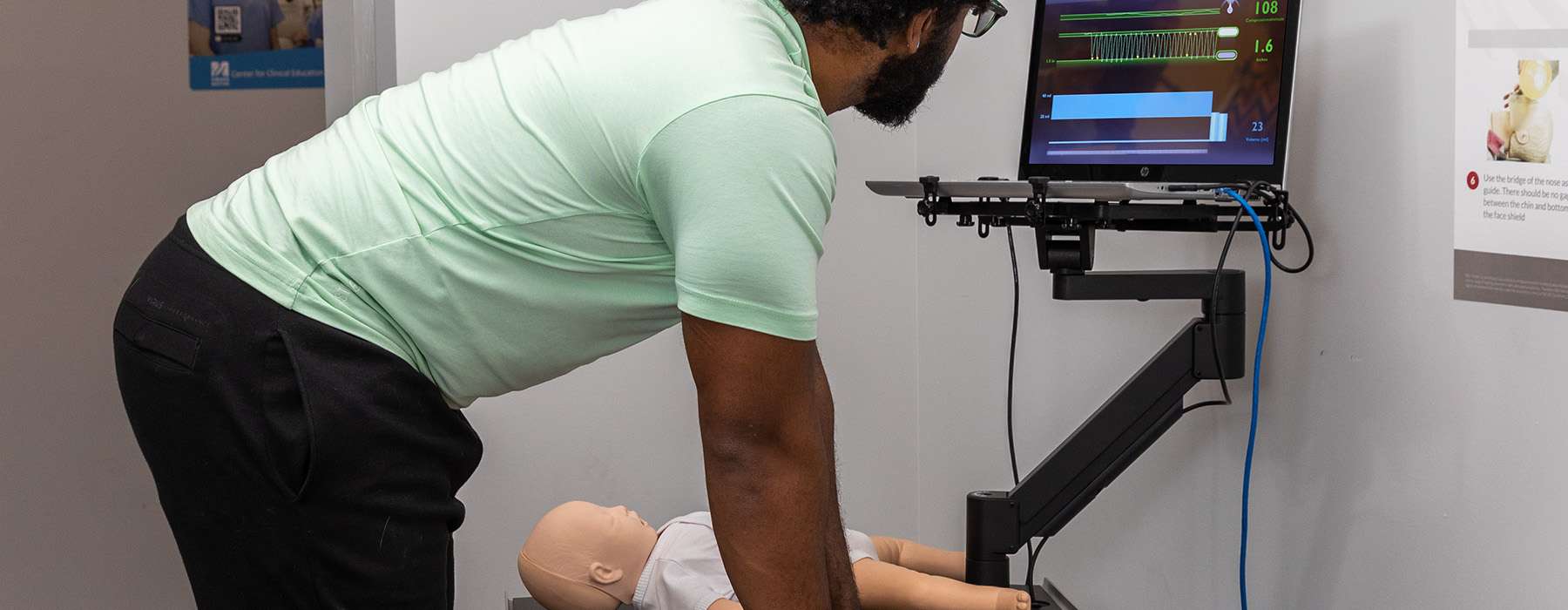
One of the biggest threats to CPR readiness is skills decay. Yet most staff are certified only every two years.
CPR skills decay within 3 to 6 months of training if skills aren’t used regularly.3
This gap creates a dangerous illusion of readiness. A coach or athletic trainer may be up to date on paper, but in a high-stress cardiac emergency, outdated muscle memory and hesitation can undermine the EAP before it is fully activated.
Approaches that emphasize more frequent reinforcement and skills assessment help close this gap. Blended learning and low-dose, high-frequency practice models allow learners to revisit core concepts regularly while maintaining hands-on competence. These approaches shift the focus from simply completing a course to maintaining readiness over time.
Training Suggestion:
Consider choosing a CPR training program that makes it easy to carry out low-dose, high-frequency training. The Resuscitation Quality Improvement (RQI®) Program is an innovative, competency-based resuscitation education program that’s fully aligned with the 2025 American Heart Association Guidelines for CPR and ECC. Learners receive an eCredential that verifies competence in high-quality CPR.
Through True Adaptive eLearning and mobile Simulation Stations for quarterly psychomotor skills activities, RQI can make sure that staff retain lifesaving skills.

When it comes to CPR training effectiveness, focusing on frequency alone isn’t enough. True CPR competence depends on realistic, hands-on practice that mirrors real-world conditions and reflects how your team actually responds during an emergency.
Effective CPR training should reinforce the team-based performance expectations embedded in an EAP:
Hands-on training with lifelike manikins helps build individual muscle memory and confidence, but its real value emerges when those skills are practiced within a team context. Real-time and summative performance feedback reinforce proper compression depth and rate while aligning individual performance with shared team expectations. This can help turn abstract guidelines into measurable, observable behaviors.
Equally important is integrating AED use into the same team-based workflow. Teams should practice clear role assignments for pad placement, shock safety, and smooth transitions between CPR and defibrillation.
With consistent practice, staff can develop the ability to respond as a coordinated, “choreographed” team.
Training Suggestion:
Aim to maximize realism by conducting training in the actual environment. Use a realistic manikin that provides detailed performance feedback, like Little Anne or Resusci Anne QCPR. Pair it with an AED Trainer that integrates seamlessly with the manikin. Or, if you prefer to use your own equipment, the ShockLink device allows your team to train with your live defibrillator.
Together, these elements will create a training experience for your team that feels authentic, immersive, and fully realistic.

If you work in athletics, you likely know that constant personnel changes are a common challenge. Graduate assistants, interns, seasonal staff, and part-time coaches rotate through programs at a steady pace. Each transition introduces variability in CPR skill levels and familiarity with the EAP.
This turnover makes it difficult to maintain consistent readiness across teams and venues. Even when departments prioritize certification, challenges remain. New staff may arrive with training completed elsewhere using different methods. CPR technique quality can vary widely, and training records can sometimes become fragmented.
Inconsistent training can lead to inconsistent emergency response. Implementing standardized onboarding and regular skills refreshers can help counter this.
Training Suggestion:
When schedules are tight, it can be difficult to find the time required to effectively manage a consistent training program. The RQI 1Stop platform can help you manage training efficiently. Monitoring and tracking course completion status and renewals can be automated through the platform, reducing the time required to manage compliance.
Programs that run on the RQI 1Stop platform include:
Both programs provide standardized skills practice and testing aligned with the 2025 American Heart Association Guidelines.

