Breaking Down Barriers to Simulation Success
Customer Story
Customer Story

Lacking the resources to grow a simulation program on their own, Pullman Regional Hospital decided to partner with Laerdal to drive their simulation aspirations forward.

Pullman Regional Hospital is an acute care hospital located in Pullman, WA.
The Challenge
Pullman Regional Hospital in Pullman, WA recognizes the importance of using simulation to prepare their providers to deliver safe, effective patient care. For over 15 years, they’ve utilized simulation to train their providers for emergencies that they don’t see every day in their small, critical access hospital.
“We do a lot of OB, but we don’t always have those OB complications that require nurses and physicians to be able to respond like it’s something they do every day,” explains Jeannie Eylar, MSN, Chief Nursing Officer at Pullman. “So simulation is key for that.”
- Jeannie Eylar, MSN
Chief Nursing Officer, Pullman Regional Hospital

But as the hospital’s services have expanded and with healthcare becoming more complex, they were finding it more and more difficult to keep their manikins up to date and train staff to run simulations.
Yet they had recently started a residency program with Washington State University, and both organizations were interested in expanding their simulation program to provide more learning opportunities for staff.
Initially, they planned to invest in a suite of new manikins – but the capital outlay was a hurdle. “Buying a family suite of manikins is extremely expensive – so I did have concerns,” explains Amber Roberts, MSN, RN, Hospital Education Coordinator at Pullman.
The Solution
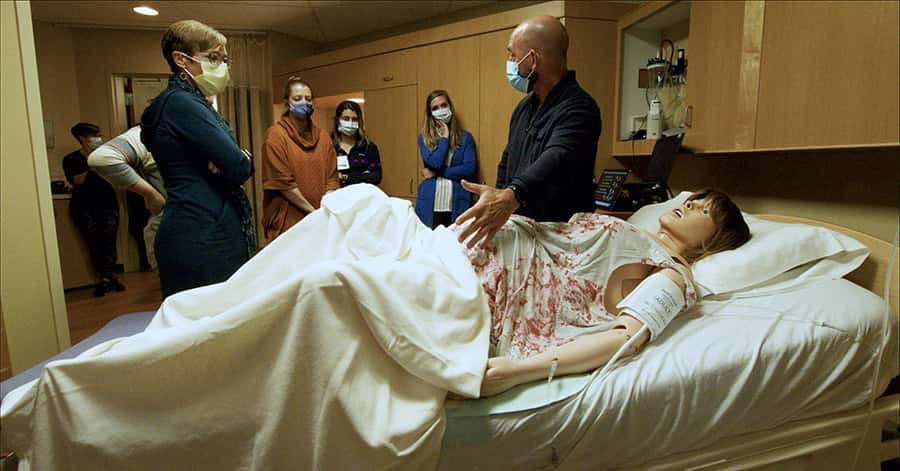
Faced with the obstacles of the cost and time associated with growing a simulation program but still determined to drive their simulation initiatives forward, Amber and Jeannie decided to try a different approach that would allow them to circumvent these challenges: partnering with Laerdal Medical through the Accelerate program.
Through this turnkey program, Laerdal would bring simulators, operators, and expert-validated scenario content directly to Pullman – providing everything needed to conduct a training session. The Laerdal team would also capture key performance data throughout the training.
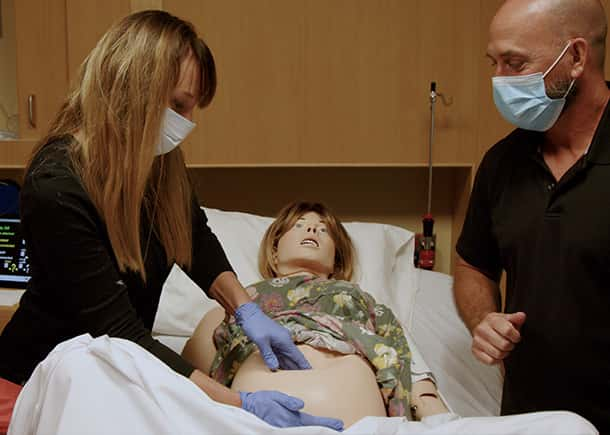
Amber and Jeannie chose a postpartum hemorrhage drill scenario for their test run of Accelerate. The performance data captured would include ACOG-aligned steps like performing uterine massage and ordering two uterotonics, as well as other key actions like ordering and receiving blood from the lab. Actions would be measured against time and the amount of blood lost. Having objective, detailed data would help identify areas the staff could improve in managing this low-frequency, high-acuity maternal emergency.
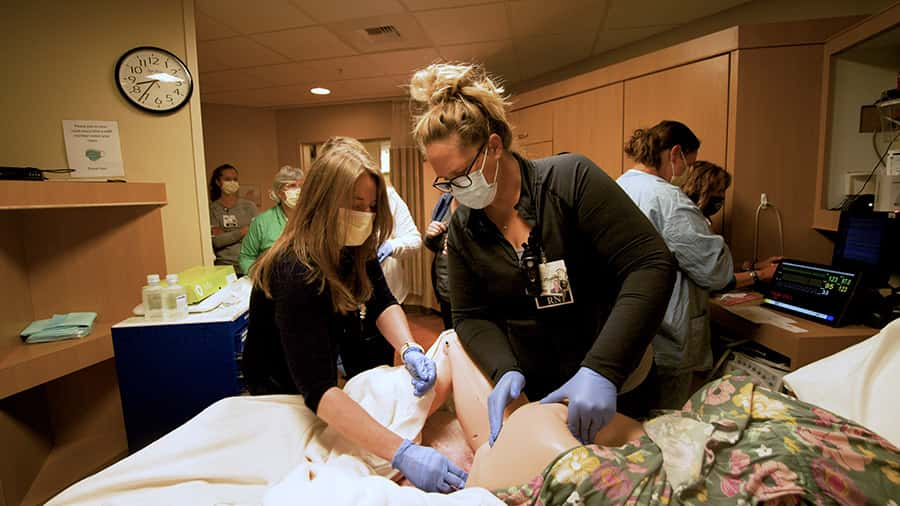
“It was extremely well received,” Amber shares. “The physicians, the nurses, RT, pharmacy – everybody involved was absolutely, completely impressed.”
“I sat in, observed, and was just totally impressed with our staff and our physicians being able to really focus on what would you do in an emergency situation like this,” adds Jeannie.
The performance data from the postpartum hemorrhage simulation scenario uncovered that there was room for improvement in the amount of time it was taking to get blood from the blood bank. This is an issue that exists in many hospitals.
“We were pretty unaware of why this was happening,” Amber tells us. But having objective data specific to their hospital gave them pathways to focus on in their Quality Assurance and Performance Improvement (QAPI) program. Using the data, they were able to set goals, make improvements, and then have Laerdal return for another Accelerate session to help them measure their progress a few months later.
The results were remarkable.
- Amber Roberts, MSN, RN
Hospital Education Coordinator, Pullman Regional Hospital

Their training efforts in obstetrics had transferred to pediatrics – indicating that the positive improvements were spreading across multiple areas of the hospital.
Having access to benchmarking data from before and after their quality improvement efforts served as tangible evidence of the ROI they’d gotten out of the Accelerate program.
After their success with the first Accelerate session, Amber and Jeannie knew they wanted to keep the partnership with Laerdal going. They’ve since invited Laerdal back to Pullman for additional sessions for training in different areas of the hospital. This includes two pediatric trainings, including a pediatric trauma, and a post-operative orthopedic complication.
Currently, they’re getting ready to run their fifth Accelerate session – their second training focused on obstetrics. “I’m so excited to do another OB simulation,” Amber shares. “I’m really hoping that we improved on our team communication – because we’ve really been pushing the training on that.”
Looking ahead, they’re planning several more Accelerate sessions in the coming year, including pediatrics, Med-Surg, ICU, OR, and ED.
- Jeannie Eylar, MSN
Chief Nursing Officer, Pullman Regional Hospital
“As I’ve gotten to know the [Laerdal] team, it’s becoming like a well-oiled machine,” Amber says. “The equipment comes … we meet the day before, set everything up. Then the next morning … off we go. The team is just so easy to work with and working with the same staff over and over again has created a lot of trust. You know your people – and there’s some safety and comfort in that.”
“We absolutely adore this program,” Amber shares. “And we’re so fortunate to have it.”
We asked Amber to share some specifics and practical tips for how she got buy-in from leadership and found success with Accelerate at Pullman.
It had everything to do with the buy-in for sure. Our CEO, CNO, [and] other clinical department leaders – we invited them to attend the different sessions for the postpartum hemorrhage. And we just kind of tucked them away in the room, and they got to physically watch how awesome it was and how the employees were so engaged, and the physicians as well, and I think that they were just absolutely sold. And I think that was key in having the administration there. That was key to the buy-in and key to how quickly – within weeks – they said, “Absolutely, we have to do this.”
There’s such a steep learning curve with dealing with manikins, which I have done. And I’ve designed sims. It is very laborious, very time-consuming – so you need a full-time staff person whose only job is sim and writing scenarios, and you need checking to make sure they’re clinically sound, etc. At least one person for our size of facility. In a larger facility, it might take 3 to 5 employees. And then, once you have your employees, they need training, and then you need to practice. It would probably take a good 6 months to maybe even a year, I would guess…if you’re starting fresh, never had any experience, etc.
We’ve been doing sim for quite a few years. So we were fairly familiar with sim, and the staff … hadn’t done it for a while [due to COVID] and all our education came to a halt just like everybody else’s. So the staff was really excited to get back into this environment because they really appreciate the learning that happens with working with your team and in situ so you get to test your systems and processes. The staff were big drivers of this, especially after [our] first experience.
I think they’re nervous at first, because they don’t want to make mistakes, and of course we encourage them. We’re like, please make mistakes during simulation. This is where we want you to make mistakes. That’s how you’re going to learn. What I really like is how the Laerdal team starts every session with a safety talk [explaining that] you’re in a safe environment, please make mistakes, this is where you’re going to learn, no one’s going to judge you … Once they get over that they’re like, “Oh, my gosh! That meant so much to me. I’m changing these one [or] two little tidbits in my practice today.”
From our data sheet that we get, our report card … we like to just focus on one or two items and not try to absorb everything we need to improve on, because that would be too overwhelming. We just grab one or two of what we see are the most important things that were pointed out, and then we work on that. I’m so excited to do another OB simulation, because I’m really hoping that we improved on our team communication – because we’ve really been pushing the training on that.
We put a lot of thought around this, and I think our key to success is getting physician champions in the areas that we’re doing the sims. So … when we did peds, we had a pediatrician champion [for example.] They kind of get the ball rolling with their colleagues as far as talking about it. We also made them sign up for sessions, and we also host sessions outside of office hours, so they don’t have to miss Clinic, for example, to attend. We tried to keep the sims about an hour, hour and a half, so that way it’s reasonable for them to pop in if they do need to leave clinic for a short amount of time. I think those things have been key.
This year we had to do some sims back-to-back or month to month, because we’re just getting started. But for 2024, we’re going to have one in February, May, August, November. That way, staff and physicians know what’s coming up and we’re going to do the same area per month. February will be pediatrics, May will be Med-Surg/ICU, or even the OR. August will be the ED. And then October, November will be the OB.
- Jeannie Eylar, MSN
Chief Nursing Officer, Pullman Regional Hospital

Simulation provides the practice opportunities that are essential to help staff be prepared to deliver optimal patient care in emergencies they don’t see often.
Enlisting the support of a simulation partner can help you achieve your simulation training goals by eliminating challenges like lack of capital outlay, time, or staff.
Simulation performance data can help establish benchmarks, identify areas for improvement, and measure progress – key areas for showing ROI of simulation training.