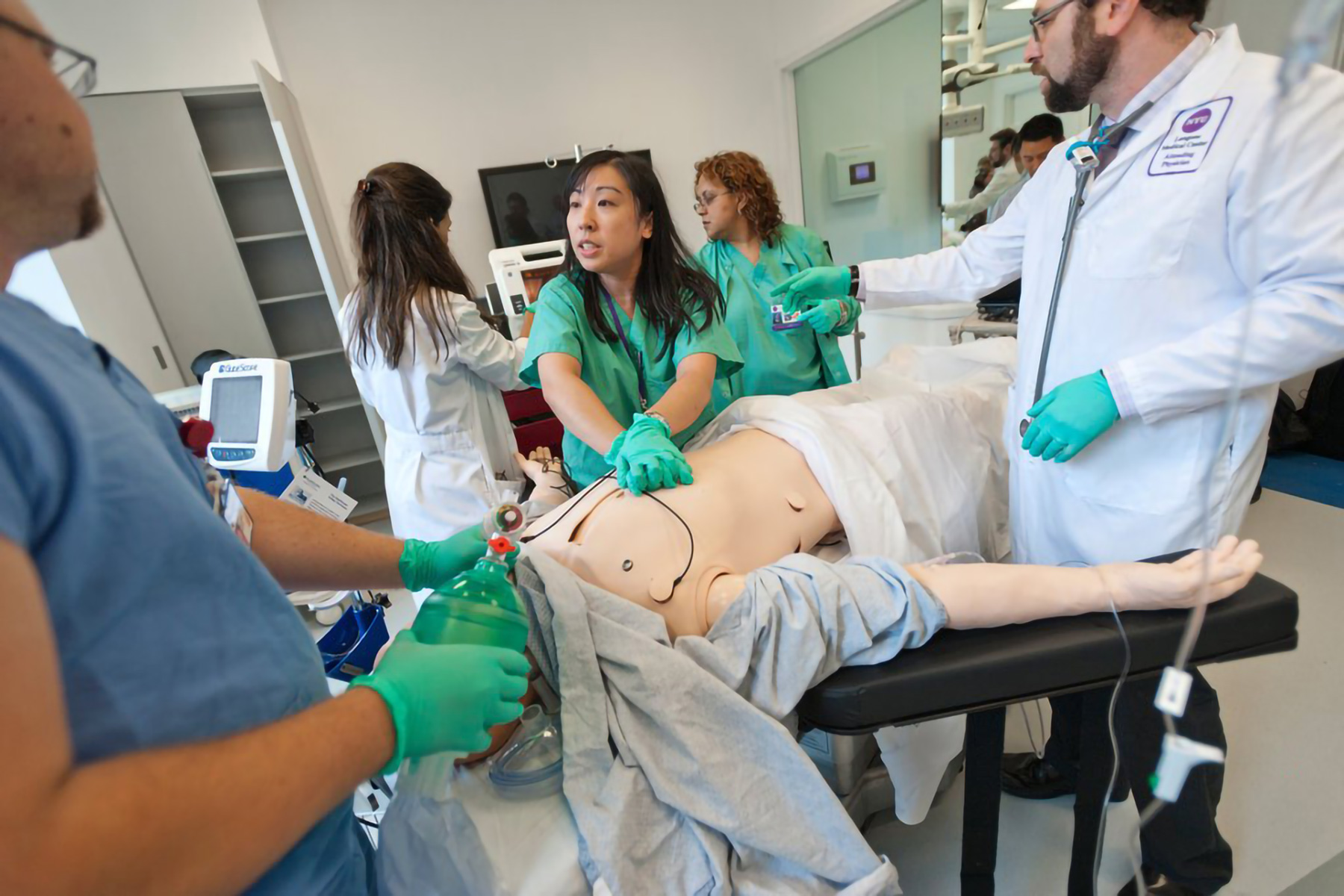
Chaos in the middle of an emergency can be off-set by command and coordination. Designated leaders, defined roles and responsibilities, and proper communication help teams stay focused and take meaningful action toward the same goal.
Simulation affords the opportunity for healthcare providers to develop these skills together, rather than in the silos of their own discipline. Bringing together an unfamiliar team can provide practice in:
- Handing off patients
- Navigating a crowded room or hallway
- Giving report to one another
- Requesting and administering medication
- Closed-loop communication skills
- Donning personal protection gear and clothing
Multi-disciplinary simulation training can effectively transfer to the bedside, even in emergencies when new team members are added and patients begin to outnumber healthcare providers.5
It’s also worth considering the psychological impact that a disaster can have on the care team, patients, and their families. Stress, emotion, and shock can all affect the overall care given to a patient. As a precaution, hospitals can work toward reducing errors in patient care by reinforcing the usefulness of the two-challenge rule and CUS (concerned, uncomfortable, safety) warnings.
In high-stress situations, it is critical that healthcare providers feel empowered to assert their concerns with one another.