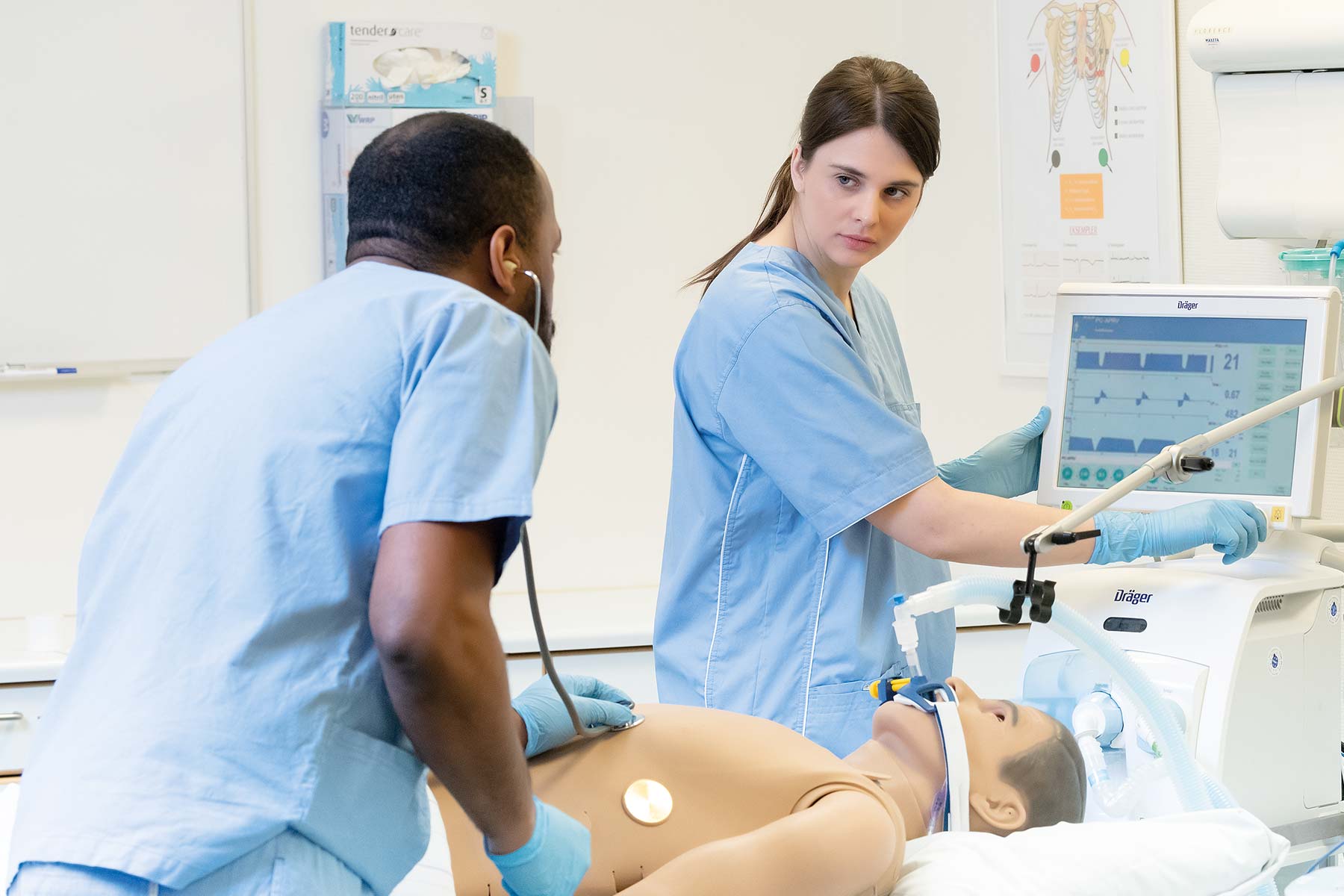
In addition to increasing the flexiblility of educational methods, some state NRBs have temporarily suspended requirements for initial licensure or for license renewal. This is in response to the rising concern that the pipeline of new healthcare workers is halting when the country needs them most.
For example, Pennsylvania has announced that nursing school graduates who have been unable to sit for the licensure exams due to cancellations caused by COVID-19 will be authorized to practice under the supervison of a registered nurse (RN).1 And, practicing RNs are being granted 90-day extensions on their RN graduate or temporary permits.
By prioritizing senior nursing students, who are closer to graduation, nursing schools are prepping them to be able to enter the field as soon as possible.
If you’re in Nursing education or any kind of healthcare training, we can help during this time. Please reach out to us. We can guide you through ways you can continue to teach virtually and offer your students the experience necessary to meet your learning requirements.