Highlights from the NLN's New Competency-Based Education Statement
5 Key Takeaways

5 Key Takeaways

If you're in nursing education, your program is likely somewhere along the path to implementing competency-based education: a model that ensures learners are graduating with "the ability to know, and also to do."1
The American Association of Colleges of Nursing (AACN)’s new 2021 Essentials: Core Competencies for Professional Nursing Education describe competency-based education as a process that shifts focus to the outputs of an educational experience rather than the inputs of the educational environment and system, putting students at the center of the learning experience.2
In February 2023, the National League for Nursing (NLN) released a new Vision Statement on this approach: Integrating Competency-Based Education in the Nursing Curriculum. In this document, the NLN shares its vision of competency-based education in nursing and translates it into actions that the NLN, nurse faculty, and nursing school leaders can undertake to help fully prepare their graduates for practice.3
Below, we highlight five snippets from the Statement and share our takeaways, along with some tips that may help you along the way as you navigate the journey of embracing competency-based education in your program.

The NLN Vision Statement implies that competency-based education puts students in the driver’s seat when mastering their competencies. Faculty become learning facilitators, or “experts in co-creating pathways for student success,” while students become champions of their own learning experience. Students will still be held to the same high standards – but now, they have more accountability for their achievement and more flexibility on their progression.
Our tip: Skills practice is one area where you can easily empower your students to take ownership of their learning – and free up faculty time and space in the process. A student-driven, digital skills practice and assessment program that works both remotely and onsite can give students flexibility as well as the freedom of unlimited deliberate practice – either independently or peer-to-peer – until they’re confident in their fundamental skills. Immediate, personalized electronic evaluations show learners areas for improvement and automated reports give faculty the insights they need on learners’ performance and utilization.
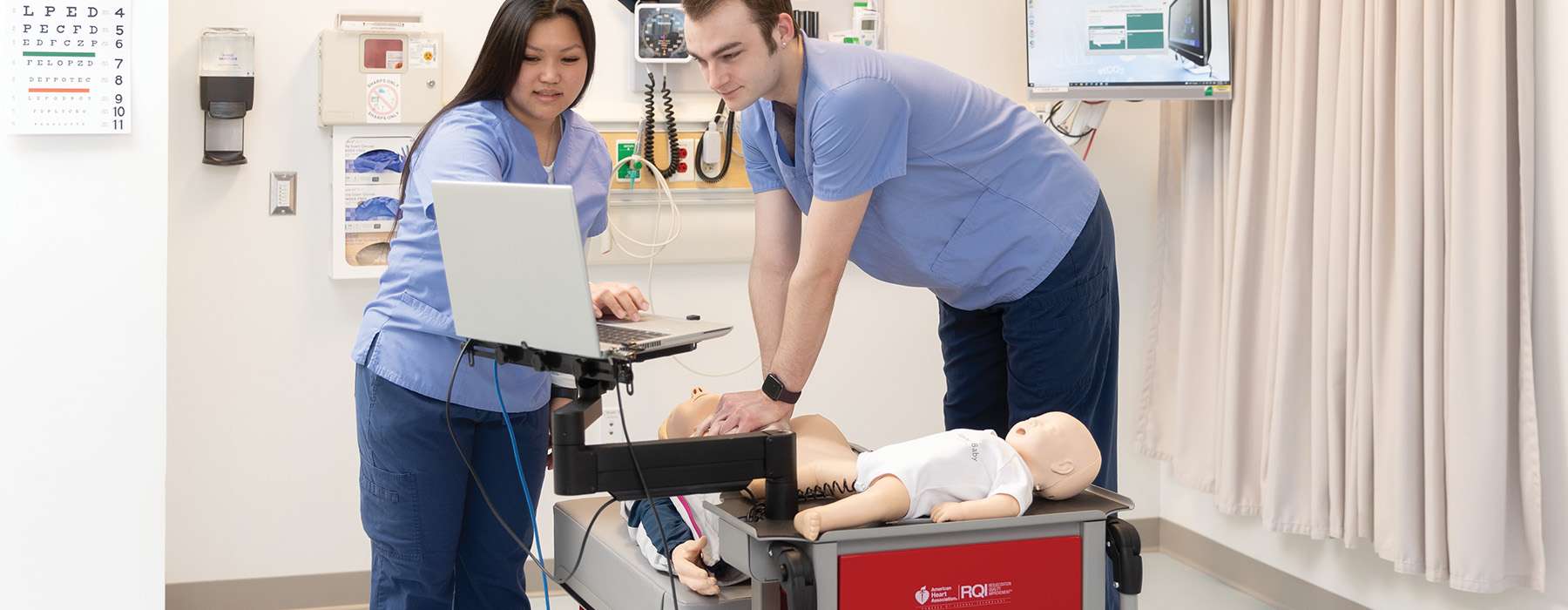
The Vision Statement points out that few competencies are performed sufficiently with just one or two learning activities. For this reason, NLN asserts, assessments should be done throughout the program – not as a one-time occurrence at the end. This means that taking a more deliberate approach of revisiting skills rather than “frontloading” them in a Fundamentals or Foundations course can help ensure students are maintaining competence across the curriculum.
Our tip: The AACN Essentials suggest creating "progression indicators" at specified points within your program of study to track students’ achievement of competencies as part of a robust program assessment plan.6 Collecting data electronically during your progression indicators with an electronic checklist for skills or a simulation learning management system (LMS) for high-fidelity simulations can help you connect the dots on students’ assessment data over time, making it easier to see their progress across courses.
Resuscitation skills decay as rapidly as three months after completing a traditional 2-year resuscitation certification7 – making this particular lifesaving psychomotor skill even more critical to revisit frequently. A quarterly, low-dose, high-frequency resuscitation education program can empower students to perform their resuscitation skills with competence and confidence. This ensures that they'll not only be practice-ready upon entry to clinical institutions, but also in their communities.

Demonstrating competencies during a formative assessment allows students to receive important feedback on areas that need improvement while maintaining a safe learning space. At some point during the course and program, NLN explains, assessment shifts to validation of students’ mastery. At the conclusion of the program, this assessment yields decisions about whether the students are prepared for practice.
Our tip: With the increased focus on clinical judgment on the NCLEX, your program is likely seeking even more strategies to foster this skill. You may want to consider virtual simulations that provide automatic, personalized feedback on clinical judgment and decision-making skills after placing students in the center of a lifelike patient encounter. Performance data, including scenario results and scores, decisions the student makes, and SBAR communications give you the visibility you need to formatively assess how well they’re grasping the learning objectives and refining their clinical judgment.
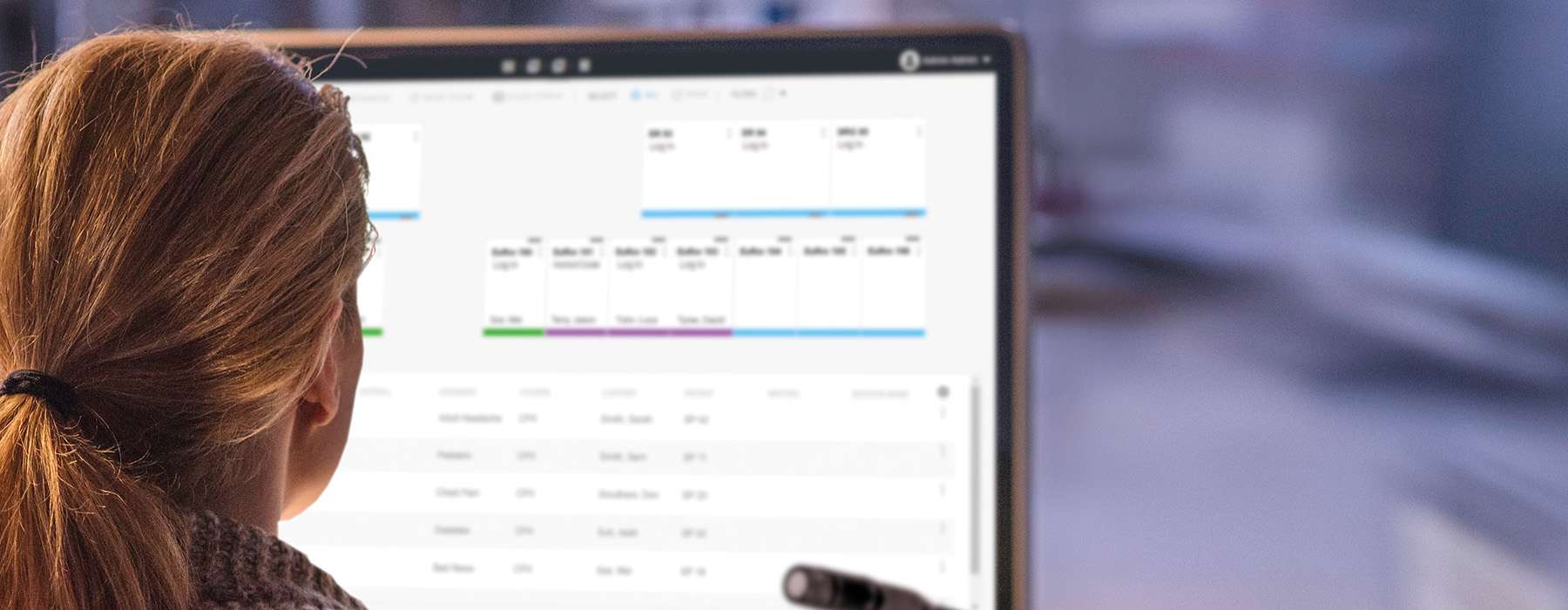
The Vision Statement explains that using student-specific learning data, guidance, and progression planning is a crucial element of competency-based education. Because progression isn’t achieved in the same manner or timeframe for everyone, some students may progress to assessment in a specific area faster than others. Having student-specific learning data allows for acceleration and deceleration as needed for students to reach mastery – even within a set course structure that may have a time limit.
Our tip: Your program is likely already collecting student data in many forms and from numerous sources. If you’re currently collecting skills or simulation performance data on pencil and paper, the shift to competency-based education may be a good time to think about implementing ways to better manage your data. Switching to an electronic skills checklist or simulation learning management system (LMS) can help you organize your data into actionable trends that will make it easier to personalize your students’ learning paths. Well-structured data can also help you reveal areas for adjustments to teaching strategies or opportunities for faculty development.
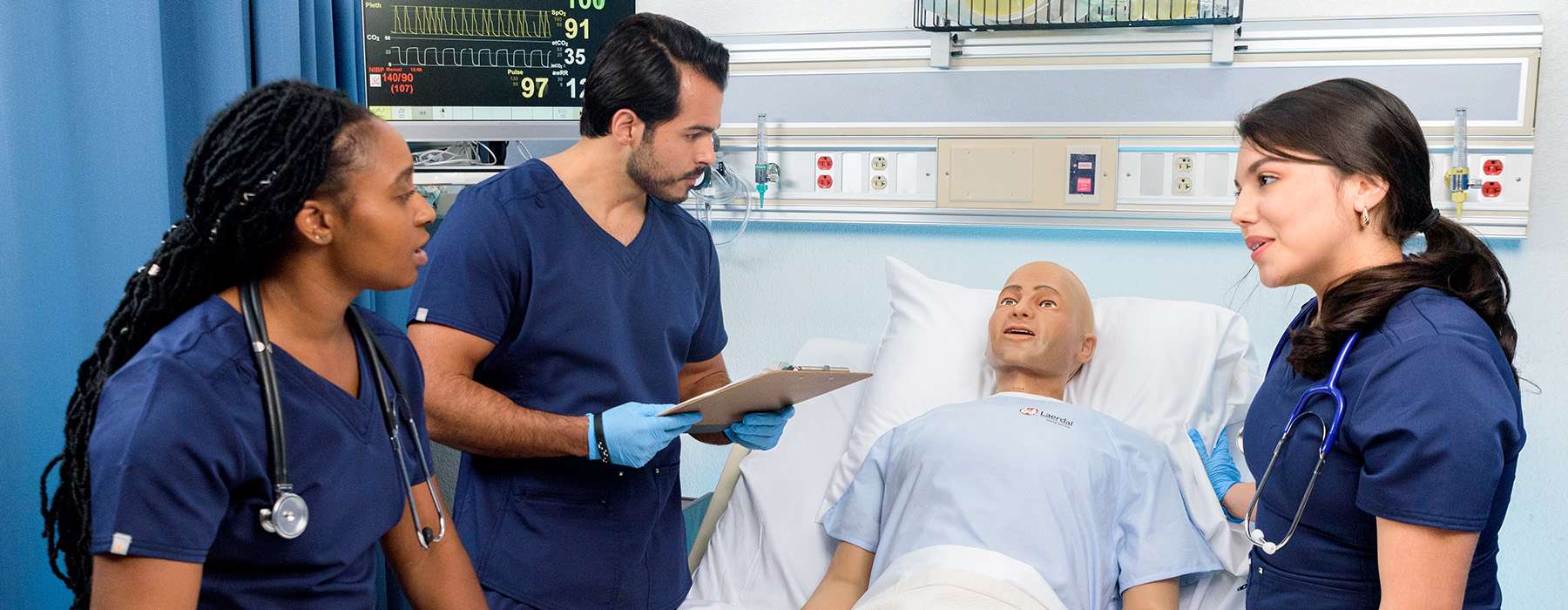
The NLN points out that most assessment methods provide data on multiple competencies. This means that with a single assessment method, you can give students the opportunity to demonstrate their abilities in several areas.
Our tip: Due to its hands-on and observable nature, simulation can allow you to assess several areas of the 2021 AACN Essentials. A single scenario can be designed to span across competencies and sub-competencies within multiple domains of the AACN Essentials, including:
The same scenario would also allow students to demonstrate several of the AACN Essentials concepts that are integrated within the competencies, such as:
And, the AACN advises that learning experiences in competency-based education must be experiential, interactive, and reflective.11 Simulation with quality debriefing encompasses all these qualities, making for an effective and engaging experience that will make learning stick.

Sign up for Laerdal Medical email updates. You can identify your interests and receive new educational content, updates, event information and more.