COVID-19 Resource Center
Complimentary simulation scenarios, safety procedures, and checklists for healthcare providers.
Our healthcare communities around the world have been dramatically challenged by the COVID-19 pandemic. Healthcare workers on the frontlines in the fight against the virus have experienced an increased risk of infection or even death. In addition, working in stressful environments increases risks to both physical and mental health making them more prone to errors which might lead to patient harm.
We lend our voice to the World Health Organization’s call to action to speak up for healthcare worker safety which requests urgent actions to recognize and invest in the safety of healthcare workers as a priority for patient safety. Because if our healthcare workers are not able to keep themselves safe, they won’t be able to keep their patients safe.

There is a 1 in 300 chance of a patient being harmed in a hospital.

1 in 4 patients are harmed while receiving primary and ambulatory healthcare.
![]()
Healthcare-associated infections occur in 14 out of every 100 patients.

More than 40 million adverse events occur to patients during hospitalization.
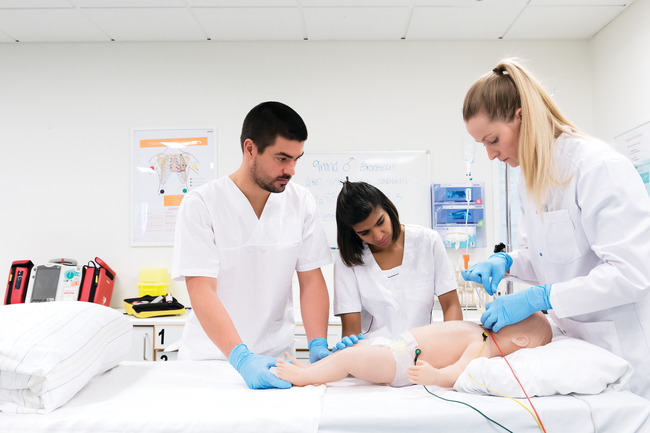
One of the biggest challenges for improving patient safety is the opportunity to practice. Clinical placement opportunities, especially within nurse education, are becoming increasingly limited as the demand for healthcare workers increases due to aging populations.
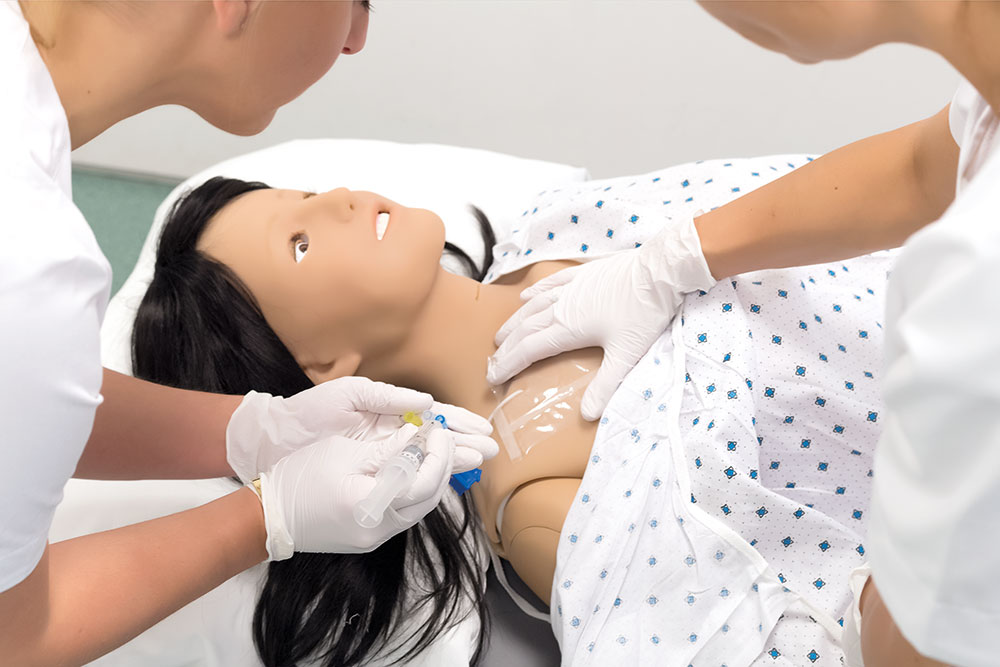
Not only is the opportunity for practice essential, but also the ability to practice safely without putting patients at risk. Simulation-based training allows students, physicians, nurses, and other healthcare providers to integrate cognitive learning with hands-on skills practice without risk to patients.

Reducing medical errors and improving patient safety are essential elements of patient care, but not the only ones. Providing optimal patient care also includes uncovering latent safety threats, facilitating teamwork and communication, and ensuring professional competency is not only maintained, but improved.
The methodology of simulation education has gained widespread recognition within the field of healthcare as a powerful tool for reinforcing clinical knowledge, improving team communication, and teaching decision-making skills. Simulation is an educational methodology, not a technology. Simulation can be used not only to teach clinical skills, but also teamwork and communication. It can also be used to standardize training, meet evidence-based guidelines, and target specific goals. There is a shift in mindset from what simulation can do to how simulation can be best used to improve patient care.
Healthcare training has traditionally relied on a “see one, do one” approach to teaching. Teaching in this context focuses on imparting knowledge. Simulation-based training makes that knowledge come alive—alive in a setting designed to imitate real clinical encounters and lifelike experiences where clinicians can refine their individual and team skills without posing risk to real patients.