Is High-Quality Simulation Your Goal?
Use the Healthcare Simulation Standards of Best Practice as your guide.

Use the Healthcare Simulation Standards of Best Practice as your guide.

If you’re looking to know more about the essentials of simulation to start or strengthen your program, the Healthcare Simulation Standards of Best Practice™ are a great place to start. Developed by the International Nursing Association for Clinical and Simulation Learning (INACSL), these standards offer evidence-based best practices in designing, conducting, and evaluating simulation experiences.
Created in 2011, the Standards were revised in 2021. "The Healthcare Simulation Standards of Best Practice are updated every 4 years, after a thorough review of the literature by an international team of interprofessional expert researchers and writers," explains Janet Willhaus, past president of INACSL.
Each of the Standards is highly detailed and contains several criteria. We've picked some short highlights from each Standard, and have shared them here. Use these highlights to get a feel for areas you believe your program can benefit from, and then investigate further by reading the full Standard(s).
It's important to note that the Standards are aspirational and meant to serve as a guide. While a number of factors might affect their full implementation in your particular organization, the Standards can help guide you in discussions with stakeholders. And, incorporating best practices help you boost consistency and efficiency in your program.
Professional Development is one of two new Standards included in the 2021 revision. “The two new Standards, Prebriefing and Professional Development, were developed because of a growing need for guidance and the developing research on these topics,” explains Suzan Kardong-Edgren, past INACSL president. The field of simulation-based education is continuing to evolve – so it’s important that your program’s simulationists evolve with it in order to ensure the best quality simulations and educational payoff for your students. This Standard emphasizes an increasing level of focus on the “pedagogy underlying the practice.”
Performing an educational needs assessment to create a well-designed professional development plan, and periodically re-evaluating the plan, are among some of the criteria included in the “roadmap” that this Standard provides. Connecting with peers and finding mentors can also help your program’s simulationists grow. Read the full Professional Development Standard here.

Tip: Laerdal's Educational Services can teach best practices for simulation training while helping you fully learn how to use our solutions to their full potential. Our Educators are former or practicing healthcare professionals who bring a wealth of knowledge and experience to what they are teaching.
Prebriefing, the second of the two new Standards for 2021, consists of preparation (pre-simulation activities) and briefing (immediately before the activity) to ensure that learners are prepared for the experience and are aware of the ground rules. Preparation might include assigning learners some nuggets of information, such as reading specific paragraphs from a text vs. a long document that they may not read.1
In addition to providing important information, the briefing component includes creating a “safe container,” or a psychologically safe learning environment where learners feel comfortable to take risks and share their feelings without fear of consequences.2 This environment is important for effective learning.
Many simulationists report that they struggle to find the time for prebriefing. However, investing in the time it takes to create and conduct a quality prebriefing will pay off in terms of what learners will get out of your simulation as a result. According to Brandon Kyle Johnson, PhD, RN, CHSE and Assistant Professor/Clinical and Simulation Director at Texas Tech University, "The tradeoff that you get as an educator is essential. When you do this work to let [learners] know about the simulation, what they’re expected to do, and set a safe container, you as an educator get a pay-off: their willingness to take personal risk."3 Read the full Prebriefing Standard here.
Good simulation-based experiences are purposefully designed to meet identified objectives and optimize the attainment of expected outcomes by mimicking what actually happens in practice. A well-designed simulation creates a story that learners can immerse themselves in and develop a picture of the patient they’re caring for. Consulting with content experts and simulationists who are well-versed in best practices in simulation education, pedagogy, and practice is key to creating a well-planned design. Measurable objectives, appropriate level of fidelity, thorough facilitation, a solid prebriefing plan, and active debriefing are also important elements. Read the full Simulation Design Standard here.

Ideally, facilitation should be conducted by a trained simulation facilitator – as specific skills and knowledge of simulation pedagogy are important for effective facilitation before, during, and after the simulation. Ultimately, facilitators should ask themselves, "How will I help the participant meet the objectives?" The facilitative approach you use should ideally be tailored to the level of learning, experience, and competency of your participants. During a simulation, use realistic cues to draw the participants’ attention to information related to the context of the scenario, or to help redirect them to obtain the anticipated learning outcomes. Examples of methods to deliver cues include lab results, moulage, and comments from patients or family members. Read the full Facilitation Standard here.
All simulation-based educational (SBE) activities must include a planned debriefing process, which may include feedback, debriefing, and guided reflection. The process should be based on theoretical frameworks and/or evidence-based concepts. The ultimate goal of the debriefing process is to promote reflective thinking. The instructor’s role in debriefing is sometimes described as being a “cognitive detective,” working to help participants explore their reflections by asking them questions to get them thinking.4 Debriefing aims to identify and resolve gaps in knowledge, skills, attitudes, and communication. A well-executed debriefing will assist in the development of insight and improve future performance. Ideally, students will transfer what they learned about navigating their thought process during your debriefing into their actual practice. Read the full Debriefing Process Standard here.

Tip: Recording your simulations can help you provide the opportunities for deep reflection that are key to effective debriefing. SimCapture can enhance debriefing by capturing video, annotations, patient monitor, and simulator data to facilitate discussion, learner self-reflection, and feedback.
Operations are the "nuts and bolts" of your program. Increased operational efficiency contributes to a smoother-running program. Ideally, a simulation program should have systems and infrastructure to support and maintain its operations. Operational role responsibilities should be accurately portrayed and could include manikin operation and programming, management and maintenance of the schedule, setup and breakdown of simulation equipment, and data collection. It’s also important to ensure operations staff receive the training they need to be competent in setting up, operating, and maintaining simulation equipment. This includes operation and troubleshooting of simulation equipment, as well as computer networking and connection of simulation IT infrastructure. Read the full Operations Standard here.
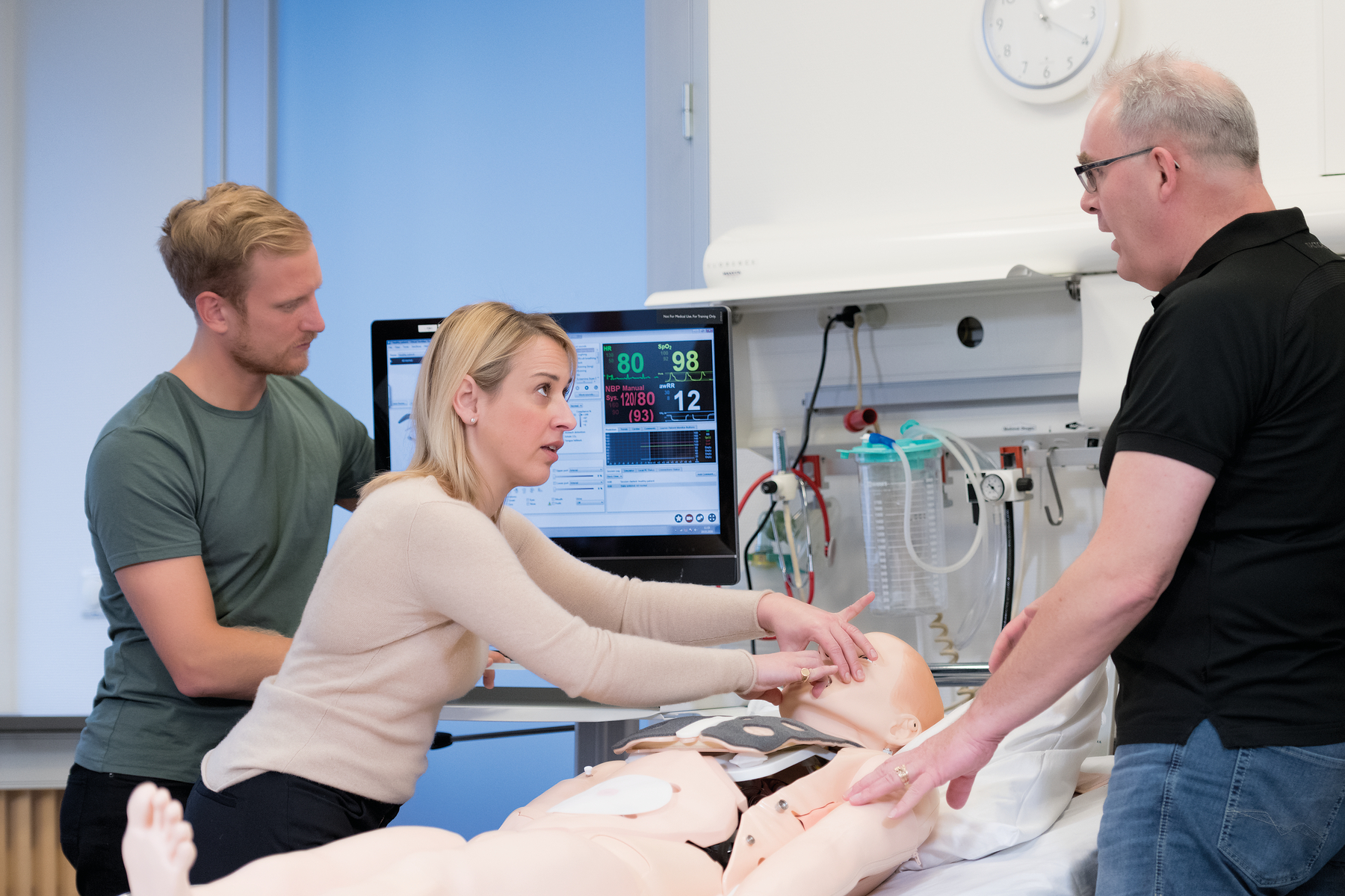
Tip: Maintaining operations is a major undertaking. You and your staff don’t have to take it all on without support. Laerdal offers Educational and Technical Services, and can even work with your IT team to set up a dedicated network for Laerdal equipment using your school’s existing infrastructure.
It’s important to clearly define the "why" behind your simulations, and what you hope to accomplish in doing them. Every simulation-based experience should originate with measurable objectives designed to accomplish expected outcomes. For example, say you want to create a simulation to teach safe medication practices. Begin by defining your expected outcome: the change in learners’ knowledge, skills, and/or attitudes that will result from participating in the simulation. In this case, your outcome would be that learners will engage in safe medication practices. Then, develop your objectives: the guiding tools that will help achieve the outcome. Your objectives could include listing the five rights of medication administration and identifying the patient using two identifiers before medication administration.5 The objectives will help guide you in determining the right simulation modality and fidelity to use. Read the full Outcomes and Objectives Standard here.

Tip: If you're struggling with which Standard to start with, this one might be a relatively easy place to begin. Try taking an existing scenario you’ve been using, and examining it against the Outcomes and Objectives Standard. Does your scenario have measurable objectives intended to meet defined outcomes? If you conclude that your approach could use some refinement, you can save time by tapping into the hundreds of expert-authored, validated scenarios available in Laerdal Scenario Cloud.
Professional integrity refers to the ethical behaviors and conduct that are expected of everyone involved throughout simulation-based experiences: facilitators, learners, and participants. Creating and maintaining a safe learning environment, practicing inclusion, and preserving confidentiality of the performances and scenario content are all important elements. Read the full Professional Integrity Standard here.
Safe, quality care is reliant on healthcare providers’ ability to work effectively together as a team. Simulation-enhanced interprofessional education (Sim-IPE) enables learners from different healthcare professions to engage in a simulation-based experience to achieve linked or shared objectives and outcomes. Basing Sim-IPE on a theoretical or conceptual framework, utilizing best practices in the design and development of Sim-IPE, and creating an evaluation plan are all ways to strengthen your Sim-IPE initiatives. If you’re already thinking about the challenges you might face in implementing Sim-IPE, you’re not alone. Many simulationists report hurdles like lack of buy-in, administrative support, resources, and time commitment/scheduling of Sim-IPE.6 However, recognition of the importance of interprofessional education has grown substantially – and simulation is an effective way to meet the need. Read the full Simulation-Enhanced Interprofessional Education Standard here.
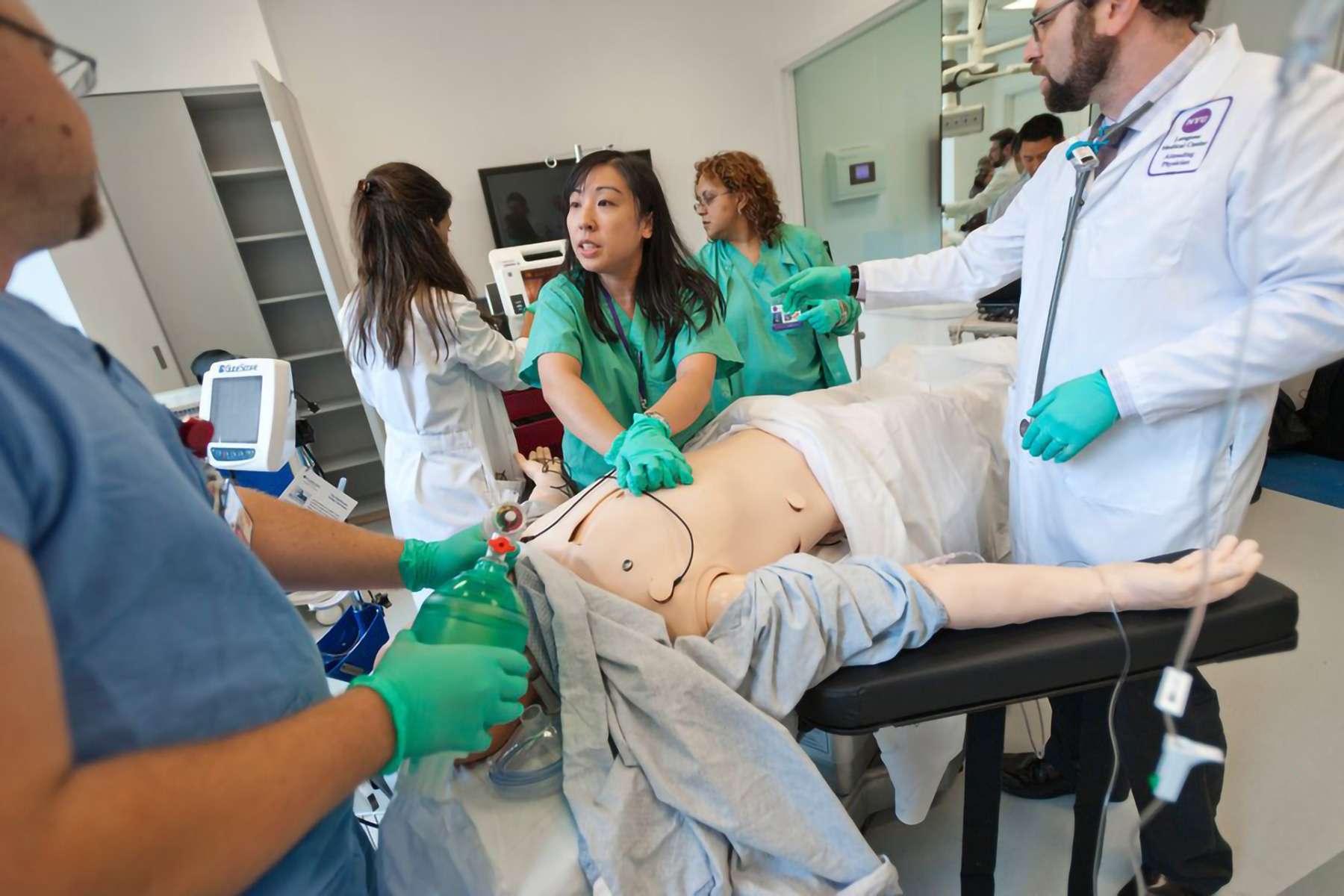
Simulation-based experiences may include evaluation of the learner. Evaluations should be directed by the objectives, outcome, and/or level of the learner. They should also be guided by their type: formative, summative, or high-stakes. The method of learner evaluation should be determined before the simulation-based experience, and it’s important to make sure learners are aware of what the expectations are. After evaluations are completed, feedback should be given to the learner. All evaluators, facilitators, and standardized patients should receive training on evaluation techniques and tools – including the usage of a valid and reliable evaluation instrument. These measures will help prevent inaccurate evaluations or assessment biases. Read the full Evaluation of Learning and Performance Standard here.
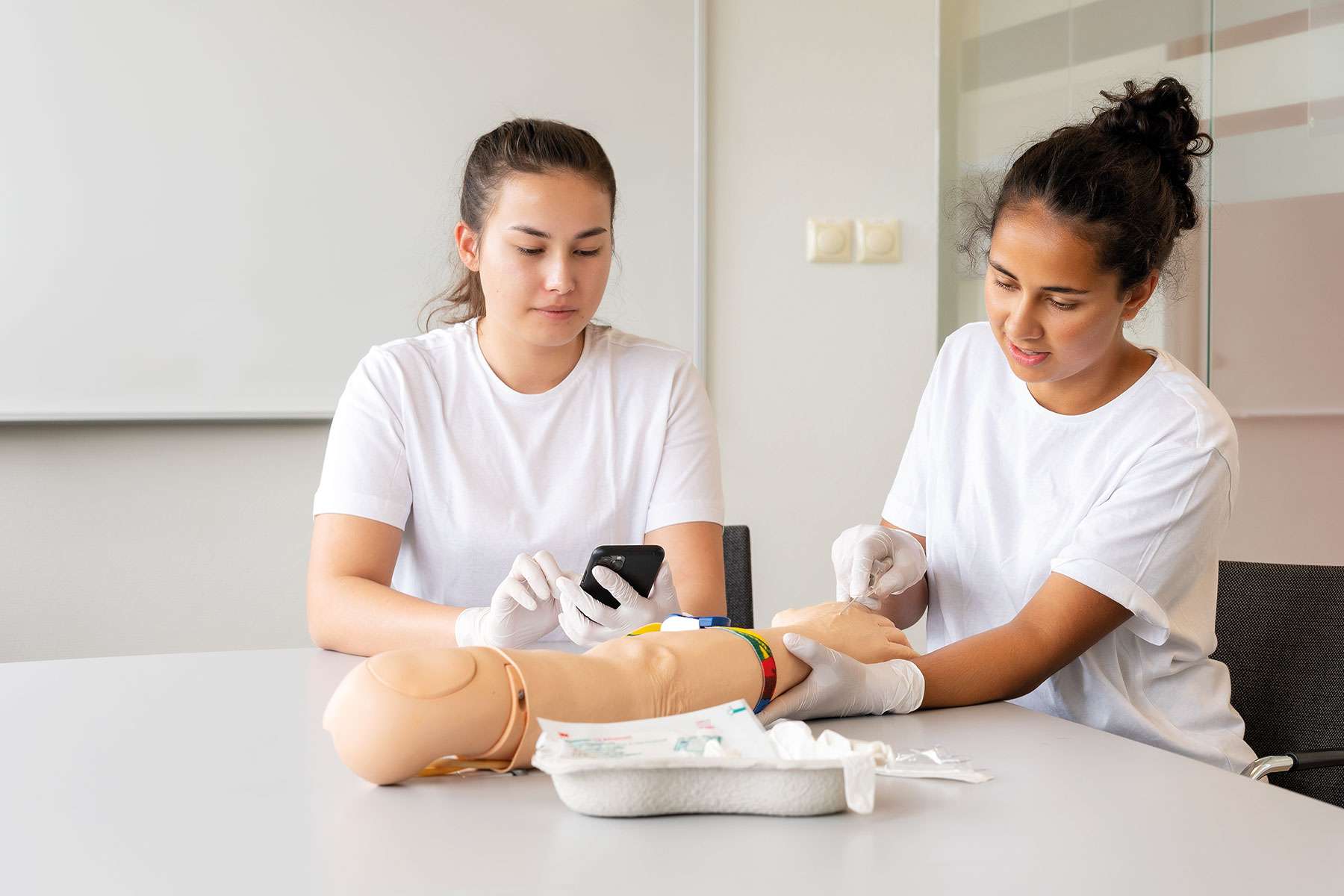
Tip: Evaluating learners during simulations and skills practice will yield a wealth of data that can give you a clearer picture of areas where you may want to focus. SimCapture can make the process easier by collecting and organizing your simulation evaluation data into actionable insights, such as uncovering a learning issue with a specific competency at the individual or cohort level. It can also reveal insights on areas for improvement in your evaluation process. A lack of inter-rater consistency in evaluation scores might point to a need for your faculty to have some additional training on using evaluation instruments effectively to ensure evaluation reliability.
SimCapture for Skills can help you evaluate learners on psychomotor skills and collect data on performance and trends over time. This will allow you to provide tailored feedback or make adjustments to your teaching approach if needed.
As you begin to further explore the specific Standards that have sparked your interest, it may be helpful to have the Society for Simulation in Healthcare’s Healthcare Simulation Dictionary within reach in case you come across any terminology you’re not familiar with. "Terms used in the SSH Healthcare Simulation Dictionary are used [in the Healthcare Simulation Standards of Best Practice] whenever possible, to standardize language and definitions for all end users," explains Laura Gonzalez, president of INACSL for 2022-2023.
SimCapture
SimCapture allows you to effectively manage, record, and assess simulation training, both on-site and in-situ.
Laerdal Scenario Cloud
Find hundreds of high-quality, expert-validated scenarios made ready for you.