Simulatie als middel om rechtvaardige zorg te bevorderen en de gezondheidsresultaten te verbeteren


Naarmate de wereldbevolking meer gediversifieerd raakt, wordt ook de patiëntenpopulatie alsmaar diverser.Dit zou zich moeten uiten in de manier waarop gezondheidsprofessionals worden opgeleid voor hun functie.
Er worden veel inspanningen geleverd om zowel diversiteit, gelijkheid als inclusie te integreren in het zorgonderwijs, zodat ongelijkheden in de gezondheidszorg kunnen worden aangepakt en de kwaliteit van de zorg en de gezondheidsresultaten van minderheidsgroepen kunnen worden verbeterd.
Het is een gekend probleem – ongelijkheden komen voor ongeacht ras, etniciteit, geslacht, leeftijd, opleidingsniveau en geografische locatie.De oplossingen zijn niet altijd even vanzelfsprekend.
Wereldwijde maatschappelijke, structurele en persoonlijke vooroordelen hebben een negatieve invloed op verschillen in de gezondheidszorg.We richten ons op de training van zorgverleners om een meer cultureel verantwoorde en bewuste zorgcultuur te bewerkstelligen.
De toepassing van simulatietraining voor zorgverleners en zorgverleners in opleiding heeft vele voordelen, zoals het opdoen van levensechte kennis, toegenomen klinisch inzicht, meer zelfvertrouwen om acute noodgevallen te behandelen, en nog veel meer.
In dit artikel bespreken we hoe simulatie kan bijdragen aan het terugdringen van impliciete vooringenomenheid en aan het beperken van de risico's voor patiënten met diverse achtergronden.Dit artikel omvat praktijkvoorbeelden en nuttige hulpmiddelen om de opleidingen binnen uw organisatie te herzien of uit te breiden, om een meer cultureel gediversifieerde leeromgeving te bevorderen en zo meer gelijkwaardige en rechtvaardige gezondheidszorg te bewerkstelligen.
De term 'ongelijkheid' wordt vaak gebruikt om verschillen tussen raciale en etnische groepen aan te duiden, ongelijkheid kent echter nog vele andere facetten - ook in de gezondheidszorg.Deze facetten, of bepalende factoren voor de volksgezondheid, zijn complex en intersectioneel.Ze moeten daarom aandachtig worden afgewogen bij het voorbereiden van zorgverleners op hun taken.Enkele voorbeelden zijn:
Race
Etniciteit
Leeftijd
Geslacht
Seksuele geaardheid
Onderwijs
Cultuur
Heritage
Religie
Geografie
Fysieke capaciteiten
Socio-economische status
Opmerking: in het kader van dit artikel zullen de termen 'diversiteit' en 'culturele diversiteit' deze vele facetten omvatten.

Als we de overkoepelende factoren die de patiëntenzorg beïnvloeden in aanmerking nemen, kunnen simulaties niet alle problemen oplossen. Ze dragen echter wel bij aan een snellere en effectievere gedragsverandering dan andere trainingsmethodes voor zorgverleners.
In vergelijking met didactische opleidingsmethodes, zoals lezingen, discriminatietraining en geactualiseerde beleidsregels, wordt simulatie beschouwd als de meest effectieve manier om de theoretische kennis ook in de praktijk te brengen. Ziekenhuizen en opleidingen voor verpleegkundigen die simulatietraining inzetten, zagen de volgende positieve effecten:1, 2, 3
Daarvoor moet u eerst en vooral het perspectief van zowel docenten als leerlingen verleggen. In plaats van uw simulatie te richten op specifieke klinische taken of strategieën voor teamwerk, moet alle aandacht uitgaan naar de patiënt. Alleen de patiënt en alle culturele aspecten die van invloed kunnen zijn op diens gezondheid.
In de gezondheidszorg lijkt dit vanzelfsprekend.De patiënt staat immers voorop. Culturele aspecten worden echter vaak over het hoofd gezien of genegeerd met de welgemeende intentie om alle patiënten gelijk te behandelen.
Het doel van simulatie voor de gediversifieerde patiëntenpopulaties is om elke patiënt individueel te benaderen.. Deze verschillen vormen de sleutel tot het leveren van betrouwbare en gelijkwaardige zorg.
Richt uw simulatiescenario op een patiëntengroep die te maken heeft met negatieve gezondheidsresultaten. Focus op gebieden waar de meeste ruimte is voor verbetering. In dit artikel categoriseren we onderzoek naar geselecteerde risicogroepen en geven we enkele suggesties voor het plannen van een gesimuleerde patiëntencasus.
Simulatie ondersteunt zorgverleners in het herkennen van interculturele vraagstukken bij de communicatie van medische informatie aan, en de behandeling van patiënten met uiteenlopende etnische en raciale achtergronden.4
U kunt leerlingen bijvoorbeeld leren om op fysiologische symptomen te letten die uniek zijn voor elke huidskleur.Of u kunt hen duiden op een aandoening waar een specifieke etnische groep vaak onder lijdt.
Tot op zekere hoogte moeten leerlingen hun vooringenomenheid opgeven bij simulatie.Door gebruik te maken van een simulator die een echte persoon voorstelt, komt het scenario echt tot leven.
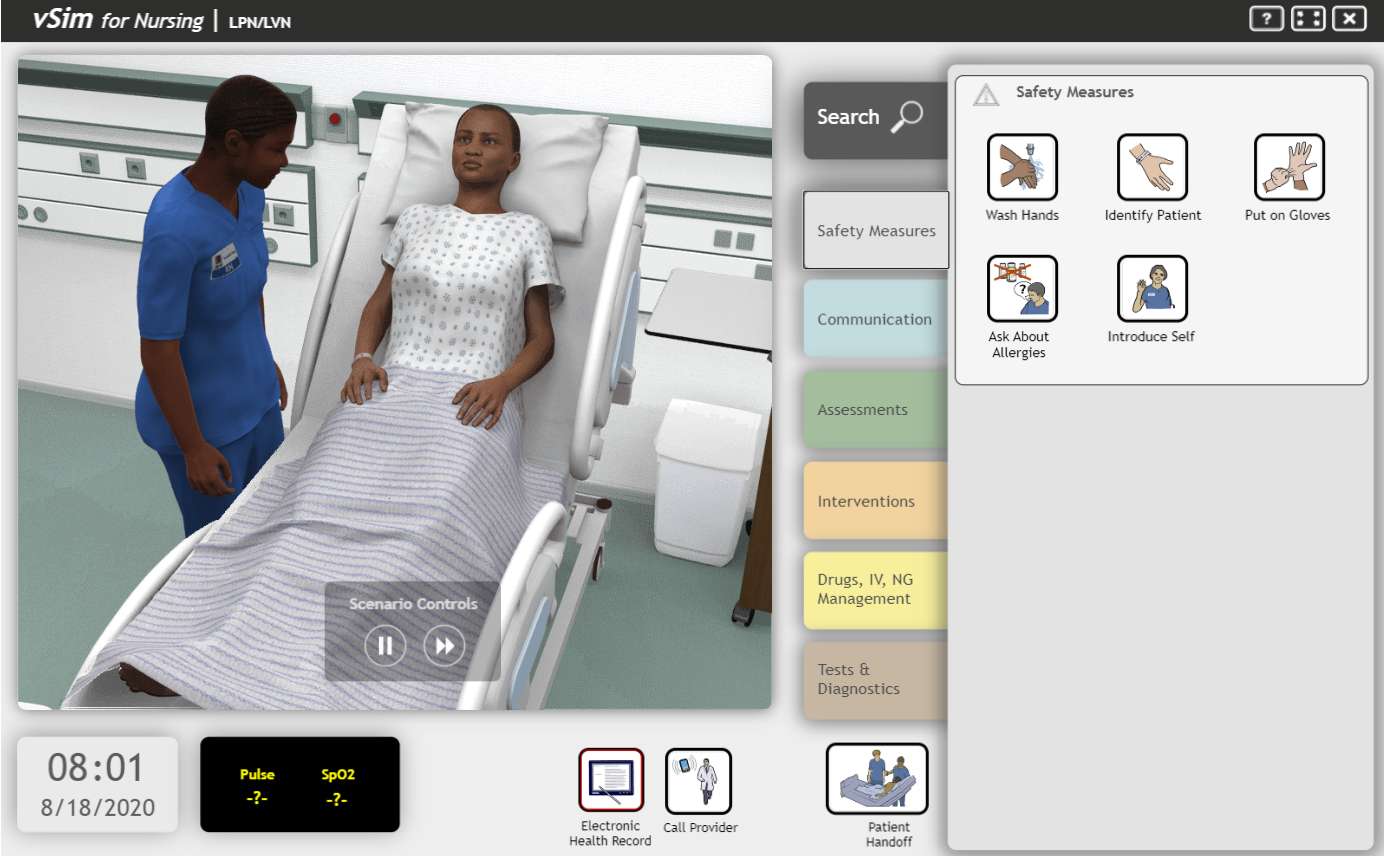
Verschillende studies tonen aan dat pijn bij zwarte vrouwen die zwanger zijn of net bevallen, vaak onvoldoende wordt behandeld.5 Bestudeer dit feit met behulp van een gesimuleerde casus: Een zwarte vrouw van 34 jaar wordt 3 weken na de bevalling, en na een zwangerschap met hoog risico, opnieuw opgenomen in het ziekenhuis vanwege stollingsproblemen en hoge bloeddruk. De bevalling vond plaats via een keizersnede en ze kampt met een pijnlijke bloeduitstorting bij de incisie en heeft ook last van hoofdpijn, troebel zicht en oedeem in haar benen.
De ontoereikende communicatie tussen zorgverlener en patiënt is een factor die vaak bijdraagt aan niet-naleving door patiënten, slechte patiëntresultaten en rechtszaken.6 In multiculturele bevolkingsgroepen kan miscommunicatie nadelig zijn voor de gezondheid van patiënten en het is van cruciaal belang dat zorgverleners geen veronderstellingen maken op basis van ras of etniciteit. Simulatie kan leerlingen vertrouwd maken met het vragen naar iemands achtergrond, hoe ze geïdentificeerd willen worden en wat hun voorkeurstaal is.
Door simulatie krijgen leerlingen ook de kans om zich vertrouwd te maken met taal- en culturele barrières. Hier volgen enkele voorbeeldstappen die u in uw scenario's kunt opnemen om het risico voor een patiënt te beperken.7
Moedig leerlingen aan om het acroniem L.E.A.R.N. te gebruiken:
Neem ook uw rol als tolk in aanmerking.
Train leerlingen om closed-loop communicatie te hanteren bij gesprekken met een tolk en de patiënt.Herhaal wat er wordt gezegd totdat de patiënt goed begrijpt wat er wordt besproken.

In de jaren negentig vestigden vrouwenactivisten de aandacht op het feit dat vrouwen vaak werden uitgesloten van klinisch onderzoek.8 Hoewel sindsdien meer vrouwen zijn opgenomen in studies, bestaat er nog steeds een 'kenniskloof' rond de gezondheid van vrouwen. Aandoeningen die vooral voorkomen bij vrouwen (zoals auto-immuunziekten, fibromyalgie en chronische pijnklachten) worden relatief weinig onderzocht. Samen met verhalen over zorgverleners die de vragen van vrouwelijke patiënten niet serieus nemen, heeft dit geleid tot een vertrouwenskloof die de perceptie van vrouwen over gezondheidszorg beïnvloedt.9
Hartaandoeningen zijn een belangrijke doodsoorzaak bij vrouwen over de hele wereld.10 Hoewel de mannelijke symptomen meer bekend zijn, vertonen vrouwen soms helemaal geen symptomen.Simuleer een vrouw van middelbare leeftijd die pijn in de kaak en keel heeft en zich misselijk voelt.Bekijk wat uw leerlingen bedenken.
Hoewel de meeste onderzoeken naar genderverschillen zich voornamelijk richten op mannen en vrouwen, is het ook belangrijk om transgenders en intersekse patiënten op te nemen in uw onderwijscurriculum.
Transgenders lopen een verhoogd risico op HIV-besmetting (met name gekleurde transgendervrouwen) en transgendermannen ondergaan vaak minder preventieve kankerscreenings.11
Voor simulatietraining die gericht is op elke vorm van genderongelijkheid zijn realistische genitaliën en anatomische kenmerken vereist, naast sterke menselijke vaardigheden voor het opbouwen van goede verstandhoudingen.Als u zich niet makkelijk voelt bij het stellen van bepaalde vragen (over bijvoorbeeld seksuele geaardheid, de gewenste voornaamwoorden van een patiënt, of ze hormonen gebruiken, enz.) kan dit een obstakel zijn voor kwalitatief hoogstaande zorg. Simulatietraining is erop gericht om dit obstakel te overwinnen.
In aanvulling op het toenemend aantal personen, lopen ook ouderen een verhoogd risico op chronische ziekten.12 Experts hebben hun bezorgdheid geuit over de toename van het aantal chronische aandoeningen en de noodzaak om multidisciplinaire benaderingen te implementeren in het beheer van patiënten.13 Aangezien ook de vraag naar thuiszorg- en persoonlijke verzorgingshulpen toeneemt, is dit een segment dat moet worden opgenomen in het continuüm voor ouderenzorg.14
Dit is precies waar simulatie het verschil maakt.Een onderzoek heeft de impact van simulatietraining gemeten op de vereiste vaardigheden voor het herkennen van dementie, valincidenten, mishandeling van ouderen en het brengen van slecht nieuws aan patiënten en hun familie.15 Door middel van een combinatie van gestandaardiseerde patiënten, simulatoren en gesimuleerde klinische documentering werden leerlingen significant vaardiger in:
Vaak wordt de sociaal-economische status (SES) beoordeeld op basis van uiterlijk alleen. Een manier om de impliciete vooroordelen van de leerlingen zichtbaar te maken, is door dezelfde simulatie twee keer uit te voeren: één keer met een dakloze man met een lage SES en één keer met een welgestelde man met een hoge SES.
Als zorgverleners onbewuste vooroordelen willen aanpakken, moeten ze leren om hun intrinsieke blinde vlekken te herkennen.Veel van deze blinde vlekken zijn het resultaat van een voorkeur voor bevestiging, wat betekent dat eerdere overtuigingen worden versterkt, terwijl nieuwe informatie die deze overtuigingen ontkracht, wordt genegeerd.
Om de constante oplettendheid en de benodigde zelfkennis aan te leren om onbevooroordeelde zorg te verlenen, kan het nuttig zijn om voorafgaand aan de simulatie de verwachtingen en basisregels te definiëren.
Hieronder vindt u een voorbeeld van hoe die richtlijnen eruit zouden kunnen zien.
Ik neem vrijwillig deel aan deze simulatie en zal daarom ten volle aanwezig en betrokken zijn en openstaan voor nieuwe kennis.
Ik ga ermee akkoord om een positieve bijdrage te leveren aan de leeromgeving en open te staan voor observaties, feedback en vragen.
Ik begrijp dat mijn overtuigingen, waarden en cultuur mogelijk verschillen van die van anderen.
Ik begrijp dat dit een gelegenheid is om verschillende manieren van zorgverlening in de praktijk te brengen, wat niet inhoudt dat voorgaande behandelingen 'fout' waren.
Ik begrijp dat sommige aspecten van deze leerervaring ertoe kunnen leiden dat ik de wereld om me heen in vraag zal stellen.
Aan het einde van de simulatie zal ik deelnemen aan een doordachte reflectie over deze ervaring.
Docenten die gebruik maken van simulaties stellen vaak dat de debriefingsessie na de simulatie het belangrijkste leermoment is. Alleen tijdens de debriefing kunnen leerlingen de informatie volledig doornemen en bespreken wat ze hebben geleerd om hun respons in toekomstige situaties te kunnen bijstellen.
Cynthia Foronda, PhD, RN, CNE, CHSE, ANEF, onderzocht en ontwikkelde de Theory of Cultural Humility, die het raamwerk presenteert om de meervoudige invloeden van divers scenario's aan te pakken.
Culturele nederigheid wordt gedefinieerd als de onderkenning van de diversiteit en ongelijkheden tussen individuen, groepen of gemeenschappen, waarbij openheid, zelfkennis, empathie, flexibiliteit, wederzijds respect en ondersteuning centraal staan, waarbij zowel de eigen persoon als de andere partij wordt betrokken om een passende benadering te vinden. Met behulp van dit raamwerk kunnen leerlingen tijdens de debriefing van de simulatie de gebeurtenissen kritisch beoordelen voor een betere identificatie en een beter begrip van diversiteit en culturele nederigheid.16
Het reflectieve proces van debriefing is een hoeksteen van de theorie inzake ervaringsleren van Kolb.17 Door een praktische ervaring (de simulatie) te vertalen in observatie en reflectie (de debriefing), kunnen leerlingen hun prestaties beoordelen en bekijken hoe ze het de volgende keer anders moeten aanpakken.
Enkele essentiële elementen van een doeltreffende debriefing zijn onder meer:
Een debriefing van een simulatiescenario bevordert het begrip van de leerconcepten, wat wordt uitgebreid door het gebruik van video-opnames.De reeks vragen van de debriefing geeft een retrospectief beeld van de prestaties van de leerlingen.Door die leerlingen videomateriaal van zichzelf en hun medeleerlingen te tonen, kan een situatie grondigere worden geanalyseerd.Dit omvat het herkennen en aankaarten van vooroordelen, stereotypering en ongelijkheden die anders mogelijk onopgemerkt blijven.
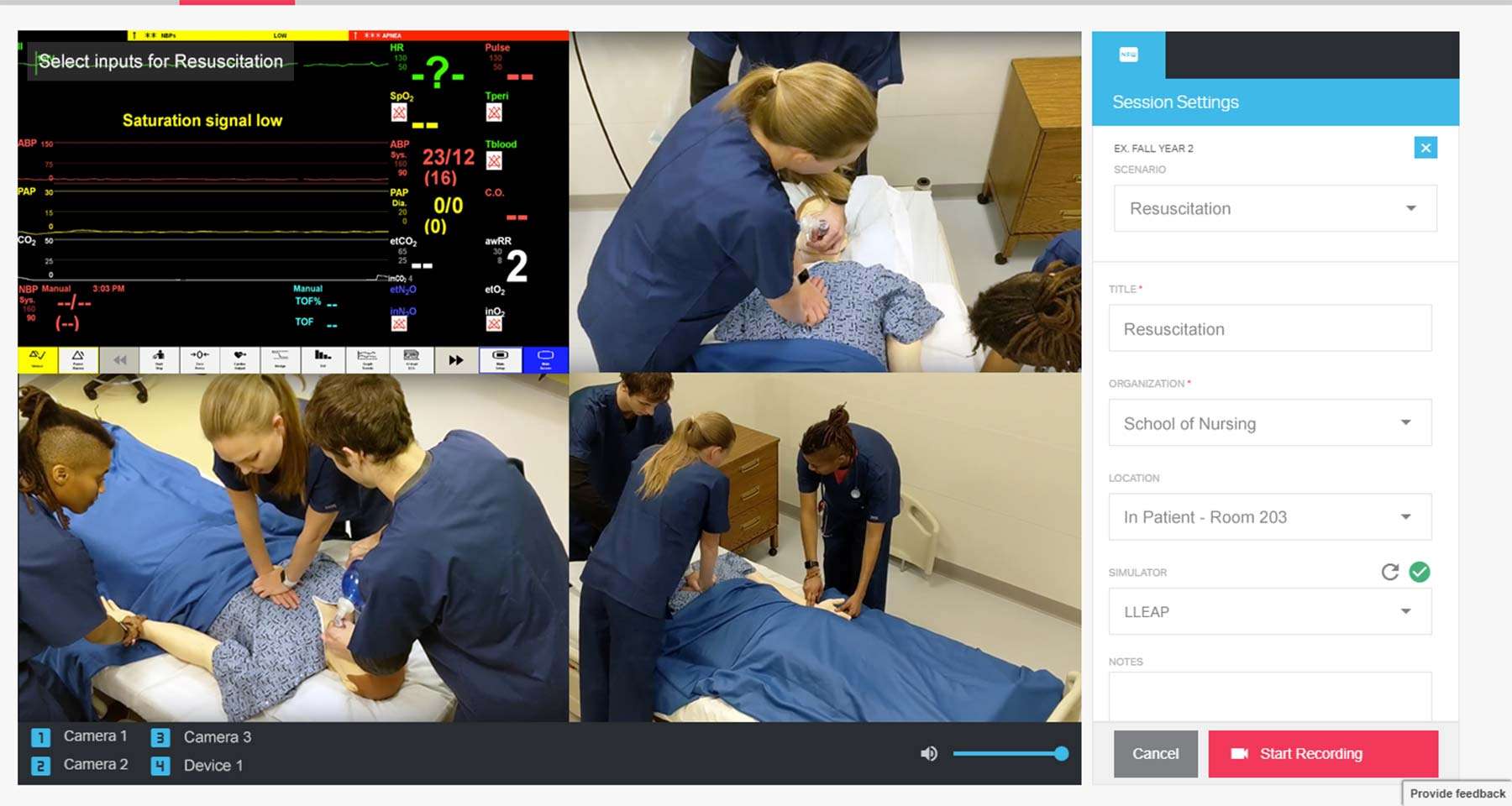
SimCapture ondersteunt u bij het beheren, beoordelen en debriefen van uw simulaties. U kunt er ook rapporten en statistieken over de prestaties mee genereren en beoordelingen van leerlingen opslaan.
In de gezondheidszorg bestaat er zowel tijdens de opleiding als de praktijk een duidelijke ondervertegenwoordiging van culturele, gendergerelateerde en etnische diversiteit.
Om daadwerkelijk in de behoeften van een gediversifieerde patiëntenpopulatie te voorzien, is training die culturele vaardigheden, culturele nederigheid en een sterk gevoel van klinische empathie ondersteunt, van cruciaal belang.

Simulatie is een krachtig instrument om de benodigde vaardigheden te ontwikkelen om alle patiënten hoogwaardige zorg te kunnen bieden.Ter afronding van dit artikel willen we u echter nog een laatste overweging meegeven: Impliciete vooringenomenheid, die gewaardborgde patiëntenzorg in de weg kan staan, kan niet op één dag worden overwonnen, noch door één enkele trainingssessie.
Het tegengaan van vooringenomenheid en het verlenen van rechtvaardige zorg vereist levenslange inspanningen en niet-aflatende oplettendheid.
Laerdal engageert zich om u oplossingen en ondersteuning te bieden om meer levens te helpen redden – voor een rechtvaardige gezondheidszorg voor iedereen in het hele patiëntenspectrum.