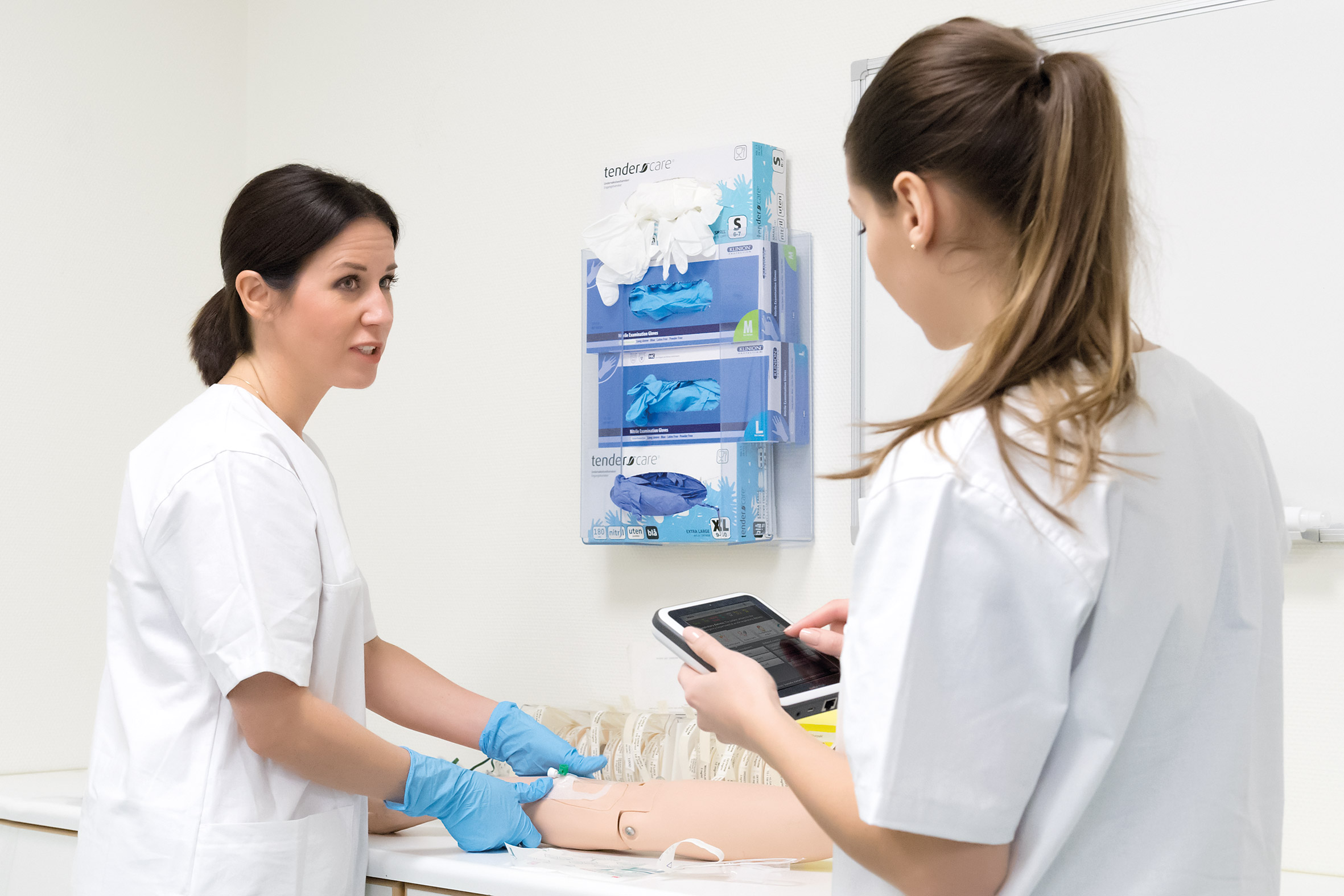
Peer-to-Peer
Tren studentene mer effektivt
I en typisk forelesningsklasse er bare 40% av studentene oppmerksomme.1 70% av studentene husker hva de hører i løpet av de første 10 minuttene av en forelesning, og bare 20% av studentene husker hva de hører de siste 10 minuttene.2 For lærere kan dette være en utfordring, for sykepleierstudenter utgjør det et alvorlig problem.
“While we teach, we learn,” sa den romerske filosofen Seneca. I tusenvis av år har utdanning kommet tilbake til dette aksiomet. Suksessen lærere har hatt med å tildele studenter til å undervise andre er kjent som Protégé-effekten. Og innenfor bruk av simulering for å bli kompetent i å utføre kliniske oppgaver, presenterer det en ideell mulighet til å ta en gammeldags læringsmetode og gjøre den moderne.
Under peer-to-peer læring opplever den tildelte læreren, protesjéen, en mye større motivasjon for å lære, noe som betyr at elevene generelt gjør mer innsats for å lære for de de skal undervise enn de gjør for seg selv.3 Det er også fordeler for de som ikke er protesjé gjennom at læring blir en sosial aktivitet der alle studentene samarbeider med hverandre for å øke sin kompetanse .4
På sykepleierskolene er det stort press for å oppnå mer med færre ressurser. Derfor har peer-to-peer blitt veldig poulært. Læringsmetoden krevet at studentene i samme situasjon lærer av og med hverandre gjennom å samhandle. I denne artikkelen vil vi forklare hvordan denne treningsmetoden kan bidra til mer effektiv trening av nye sykepleiere.
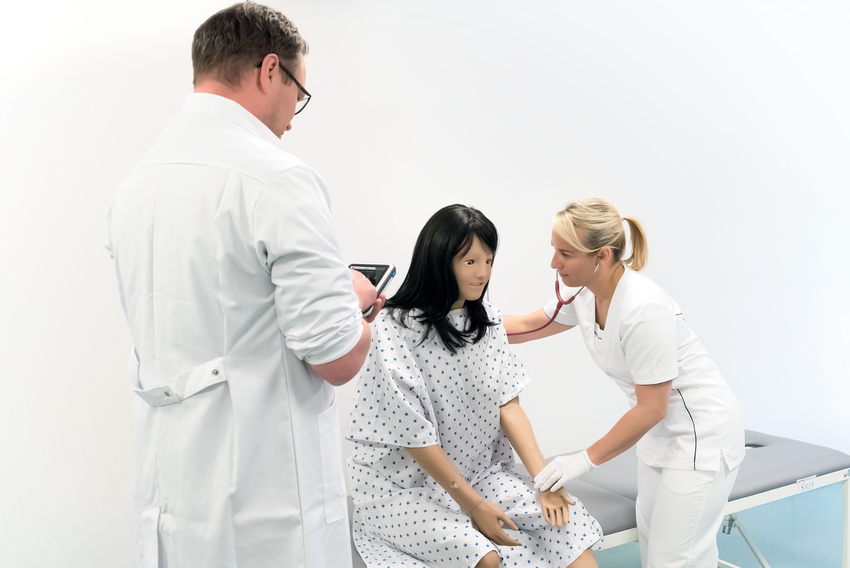
Skap flere kliniske kvalitetsopplevelser med færre ressurser
Ofte er klassene på en sykepleierskole store og preget av klasseromsundervisning. Det begrensede antallet en-til-en eller små gruppeinteraksjoner for å utvikle ferdigheter kan ha en negativ innvirkning på elevene. Studentene bruker mindre tid på å øve på ferdigheter på fritiden, en grunn til dette kan være at de allerede bruker mye tid og energi på studiene.
Peer-to-peer læring kan bidra til å møte studentenes behov for ferdighetstrening. En studie fant at studenter som brukte peer-to-peer metoden opplevde økt selvtillit og støtte i å utføre psykomotoriske ferdigheter.5 En annen studie antydet at prestasjonene til de som lærte gjennom peer-to-peer ville være betydelig bedre enn de som hadde en tradisjonell økt.6 Begge funnene peker på peer-to-peer som en måte å forbedre studentresultatene på.
Hvis organisasjonen din har vanskeligheter med å få nok ressurser fra fakultetet, kan peer-to-peer læring være en alternativ metode som kan være til hjelp. I denne tilnærmingen er fakultetet tilretteleggere som setter forventninger, deler ut oppgaver og følger med på studentenes interaksjoner. Men det er studentene selv, spesielt de som er mer erfarne, som leder ferdighetstreningen, observerer andre studenter og gir detaljert tilbakemelding og veiledning gjennom scenarioene.
Vil du vite hvordan du kan lykkes med peer-to-peer læring?
DO's & DON'Ts sjekkliste
Ved å bruke denne sjekklisten kan du sørge for at fakultetet skaper et godt miljø som maksimerer fordelene med å lære av og med hverandre.

Engasjer studentene gjennom teamarbeid, kommunikasjon og tilbakemelding
Det sies ofte at millennumsgenerasjonen sitter klistret til telefonene sine – og en nylig undersøkelse viste at det er sant! 39% av milleniums (født mellom 1981 og 1996) innrømmer at de samhandler mer med smarttelefonene sine enn med ektefeller, foreldre, venner eller kolleger.7 I en tid med økt skjermtid kan studentene oppleve mindre ansikt til ansikt tid med andre studenter og deres instruktører. Tid til diskusjon og gruppeøvelser kan være begrenset, og studentene kan begynne å føle seg isolert i studiene.
Peer-to-peer kan gi det personlige engasjementet som milleniums ønsker. Forskningsresultater viser fordeler med peer-samarbeid som støtter overgangen fra studie til klinisk praksis, inkludert å forberede studentene til å veilede i det kliniske miljøet og redusere mangel på selvtillit.8 Eksperter mener også at peer-to-peer gir en følelse av tilhørighet som kan hjelpe elevene til å håndtere akademisk stress. Studentene vil ofte søke råd og veiledning fra sine jevnaldrende, spesielt når de presenteres med nye konsepter. Og slik sosialisering har vist seg å styrke læringsprosessen.9
I tillegg til de psykologiske fordelene, ser studentene også kognitiv forbedring med peer-to-peer læring. En studie fant at denne læringsformen blant sykepleierstudenter førte til økt klinisk nøyaktighet og færre praktiske feil.10 En grunn til dette kan være at når studentene bruker peer-to-peer læring, blir de ansvarlig for sin egen innsats samt for å hjelpe andre studenter. Dette fører til at de blir mer engasjerte i emnde de lærer om.
Med peer-to-peer læring vil studentene engasjere seg for å oppnå de beste resultatene. Ved å gjenta en ferdighet eller scenario flere ganger, kan de trene i et trygt miljø til de føler seg kompetent.

Bedre avkastning for organisasjonen og studentene
I dag ser mange høyskoler etter alternative tilnærminger til tradisjonell klasseromundervisning. Dette kan skyldes budsjettkutt, større student kull og økte krav til de ansatte.11 En fordel med simulering som ekspertene fremhever, er at det gir god avkastning på investeringene. Det er viktig å huske at avkastning ikke bare kommer fra scenario-basert simulering, men også fra ferdighetstrening.
Peer-to-peer kan bidra til å spare tid. Ved å la elevene vurdere hverandres ferdighetsnivå i stedet for læreren, kan flere treningsøkter gjennomføres samtidig uten å gå på kompremiss med kvaliteten. Faktisk har sykepleierstudenten uttalt at tilbakemeldingene de får fra medelevene sine er mer nyttige enn tilbakemeldingene fra læreren.12
I tillegg kan peer-to-peer bidra til å spare ressurser. Simulatorer og personalet som betjener dem kan være dyre, derfor kan det være mer fordelaktig å innføre ferdighetstrening først. Studentene får grunnleggende ferdigheter og kunnskaper, og dette kan hjelpe med å bestemme når en investering i fullskala simulering er nødvendig.
Det er også avkastning for studentene. En studie har funnet at peer-to-peer bidrar til utviklingen av profesjonelle ferdigheter, som for eksempel tilbakemeldingsteknikker, lederegenskaper og selvstendig læring.13 Studenter investerer mye i utdanningen sin, og hvis de opplever at de har hatt en positiv opplevelse og fått avkastning, kan dette reflektere positivt på skolen.
Hvordan kan peer-to-peer læring hjelpe?
International Council of Nurses (ICN) spår at det vil være behov for over 13. millioner sykepleiere over hele verden innen 2030 for å møte den kommende mangel på sykepleiere.14 På grunn av ressursmangel kan ikke skolene øke antall studenter.15
Peer-to-peer læring er en måte skolene kan møte utfordringen fremover. Selv om det ikke er ment å erstatte tradisjonell klasseromsundervisning eller scenario-basert simulering, tilbyr den et komplementært og svært verdifullt opplæringsalternativ. Fakultetet kan maksimere sin begrensede tid mens studenter (og deres fremtidige pasienter) nyter fordelene med gjentatt og sikker ferdighetstrening.

References:
- Cameron P., Giuntoli D. (1972). Consciousness sampling in the college classroom or is anybody listening? Intellect 101, 63–64.
- Ibid
- Billett, S. (2011). Learning in the circumstances of work: The didactics of practice. Education & Didactique. Retrieved from https://journals.openedition.org/educationdidactique/1251
- Dreon, O. (2016). The protégé effect. The 8 Blog. Retrieved from https://the8blog.wordpress.com/2016/03/08/the-protege-effect/
- DeBourgh, G.A. & Prion, S.K. (2017). Student-directed video validation of psychomotor skills performance: A strategy to facilitate deliberate practice, peer review, and team skill sets. International Journal of Nursing education Scholarships, 14(1). DOI: 10.1515/ijnes-2016-0020
- El-Sayed, S.H. (2013). Effect of peer teaching on the performance of undergraduate nursing students enrolled in nursing administration course. Journal of Nursing Education and Practice, 3(9). Retrieved from http://www.sciedu.ca/journal/index.php/jnep/article/view/2822
- Hill, C. (2016). Millennials engage with their smartphones more than they do actual humans. Market Watch. Retrieved from https://www.marketwatch.com/story/millennials-engage-with-their-smartphones-more-than-they-do-actual-humans-2016-06-21
- Carey, M.C., Kent, B., & Latour, J.M. (2016). The role of peer-assisted learning in enhancing the learning of undergraduate nursing students in clinical practice: A qualitative systematic review protocol. JBI Database of Systematic Reviews and Implementation Reports, 14(7), 117-123. Retrieved from https://www.nursingcenter.com/journalarticle?Article_ID=3629808&Journal_ID=3425880&Issue_ID=3629148
- Stone, R., Cooper, S., & Cant, R. (2013). The value of peer learning in undergraduate nursing education: A systematic review. International Scholarly Research Notices: Nursing. DOI: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3649279/
- Ravanipour, M., Bahreini, M., & Ravanipour, M. (2015). Exploring nursing students’ experience of peer learning in clinical practice. Journal of Education and Health Promotion, 4. DOI: 10.4103/2277-9531.157233
- Ahmad, I.M. & Mohamed, H.E. (2018). The effect of peer learning vs. traditional learning on knowledge and clinical performance of critical care nursing students. Journal of Education and Practice, 9(8). Retrieved from https://www.iiste.org/Journals/index.php/JEP/article/download/41661/42885
- Ibid
- Burgess, A., McGregor, D., Mellis, C. (2014). Medical students as peer tutors: A systematic review. BMC Medical Education, 15, 115. DOI: 10.1186/1472-6920-14-115
- International Council of Nurses. ICN; Geneva: 2021. ICN Policy Brief- the Global Nursing Shortage and Nurse Retention. [Internet] https://www.icn.ch/system/files/2021-07/ICN%20Policy%20Brief_Nurse%20Shortage%20and%20Retention.pdf
- Kavilanz, P. (2018). Nursing schools are rejecting thousands of applicants – in the middle of a nursing shortage. CNN Business. Retrieved from https://money.cnn.com/2018/04/30/news/economy/nursing-school-rejections/index.html